On April 20, 2021, 38-year-old Sona Agarwal* was told her breathlessness might be a symptom of coronavirus-induced pneumonia that only a CT scan could confirm. It took three days for her COVID-positive husband to find an ambulance to take her to a laboratory for testing.
“My doctor saw the scan and recommended immediate hospitalization,” she says. Another two days went before they found a bed in a remote Delhi suburban hospital. Agarwal is now recovering in hospital but says she is traumatized.
Every day, she says, at least four patients, after gasping for oxygen that is in short supply, die in her vicinity. “To be so sick and find that your country’s health infrastructure has completely failed has been unsettling, to say the least,” she says from her hospital bed.
“From things we once took for granted like organizing home testing, getting doctor appointments, and buying medicines – to things we’d never done before like hunting for ambulances and hospital beds and arranging for our own oxygen concentrator, the whole experience has been a nightmare.”
Daily COVID-19 cases fell to below 10,000 In February 2021, and two vaccines were to be rolled out by March 1. Many thought the worst was over. But a deadly second wave has seen the daily caseload explode to over 400,000 in the beginning of May. The country’s medical infrastructure in disarray, Prime Minister Narendra Modi’s government is facing criticism for allowing large crowds to gather for religious festivals and election rallies in various parts of the country.
“The health system is completely overwhelmed as a result of a lack of foresight and planning,” says Inayat Singh Kakar, a public health researcher with global health network Jan Swasthya Abhiyan (People’s Health Movement India). Like Agarwal, people across the country are feeling abandoned by the state as they struggle to cope with the deadly second wave of COVID-19.
“Today, patients are dying not just from being infected, but also from the lack of oxygen, medical help, and hospital beds,” says Dr. Harjit Singh Bhatti, national president of Progressive Medicos and Scientists Forum (PMSF), a group of doctors which advocates for ethics and compassion in medicine. “Although the central government and states had all of last year to prepare for the imminent second wave, oxygen production wasn’t stepped up. Hospital capacities were not increased. And the unexpected ferocity of transmission of the second wave has brought the system to its knees.”
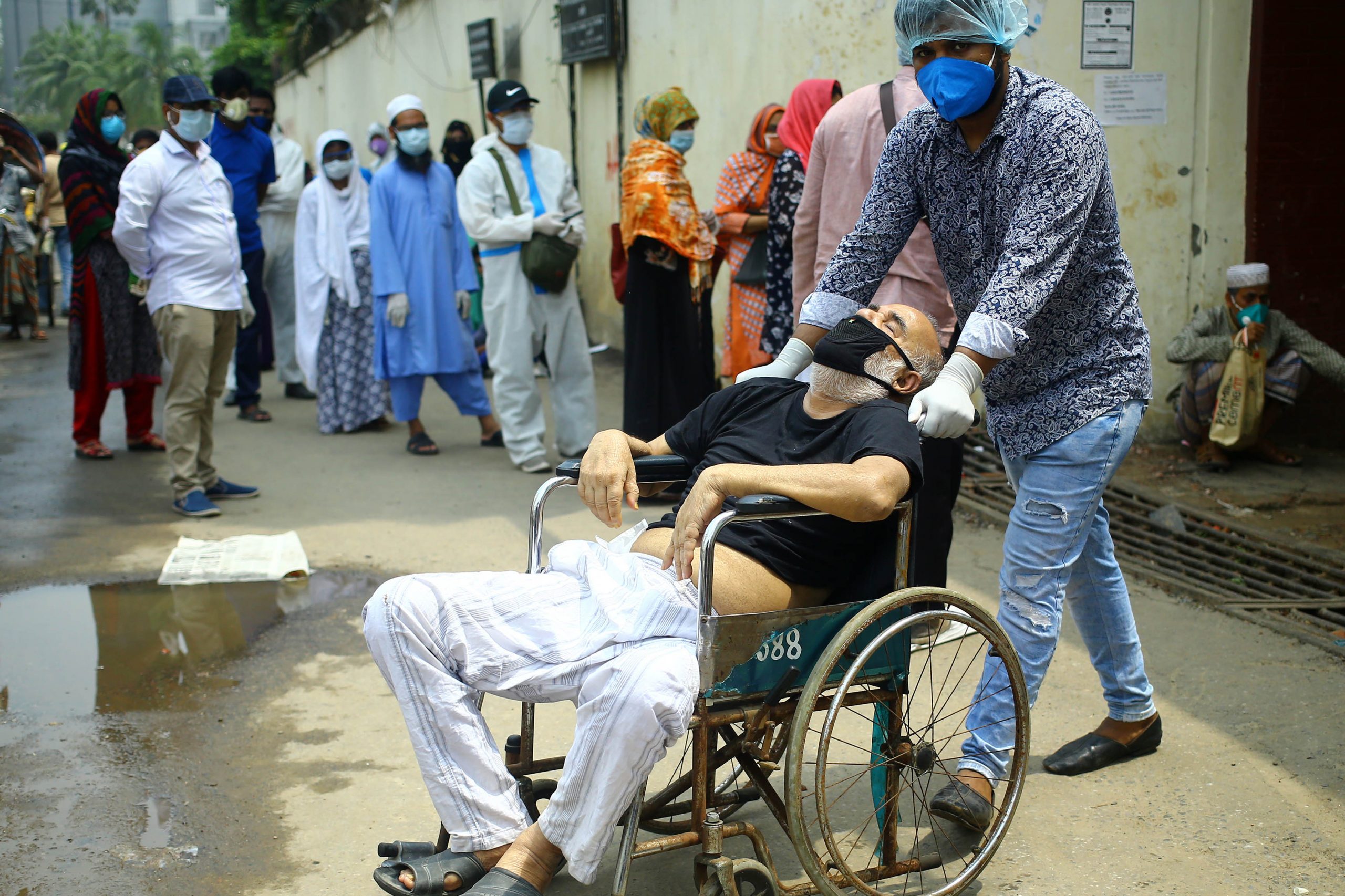
A dire shortage of medical oxygen and hospital beds, among other systemic cracks in India’s healthcare system, has exposed a dark, glaring reality—the Modi government’s inability to tackle the pandemic.
Exploding caseloads, exhausted medics
With exploding caseloads in several states, especially following large public gatherings such as the annual Hindu pilgrimage Kumbh Mela, and election campaigns in southern states of Kerala and Tamil Nadu and the eastern states of Assam and West Bengal, doctors say they are swamped by hordes of patients coming in with respiratory distress. “There used to be two doctors for every five patients in our ICU before the pandemic,” says Dr. Siddhartth Taara, general-secretary of Resident Doctors’ Association of Delhi’s Hindu Rao Hospital. “Today, 10 critically ill patients are being treated by a single doctor!”
An exhausted Dr. Bhatti, who practices in a private Delhi hospital, says their caseload has seen a four-, even five-fold increase. “This time round, they’re younger and sicker than patients in the first wave,” he says. Nurses in Maharashtra, India’s second most populous state, report working 10- to 12-hour shifts in the same personal protective equipment suits.
“Nurses who were tired and overworked anyway during the first wave are now exhausted beyond reason,” says Swati Rane, member of the Mumbai chapter of Jan Swasthya Abhiyan (People’s Health Movement). “The high mortality rates in the second wave have contributed to their stress.”
Like Dr. Taara, nurses and doctors have been falling sick every day as the second wave rages. On April 27, the capital’s Lok Nayak Hospital reported the death of a third medical staff for the third consecutive day. Many hospital staff say that their hospitals are so overcrowded that they are not even assured of beds if they fall ill. Adding to their insecurity, the Central government’s special insurance scheme that promised approximately US$67,700 to the family of every health worker who dies of COVID-19 while on duty has now lapsed and no new scheme has been announced yet.

Dr. Harjit Singh Bhatti, national president of Progressive Medicos and Scientists Forum, during one of his medical field visits. He says “patients are dying not just from being infected, but also from the lack of oxygen, medical help, and hospital beds.”
Gasping for oxygen
A large part of the infrastructural failure underpinning the new wave is the shortage of oxygen, which many medics like Dr. Bhatti allege has caused the majority of recent deaths.
“As a nurse/patient advocate, I’d never in my wildest dreams thought I’d see so many patients die in hospital for the lack of oxygen!” says Rane. In Maharashtra, she observes that the demand for hospital beds has been compounded by the reduced availability of oxygen concentrators and cylinders needed for home care.
 Across the country, charities offering oxygen support and compiling lists of oxygen suppliers are swamped too. Since the first wave in 2020, a couple of Sikh religious groups under the umbrella of Covid Fight Support Saanjh (CFSS), a religious charity, have been soliciting oxygen cylinders, beds, even food deliveries using private donations.
Across the country, charities offering oxygen support and compiling lists of oxygen suppliers are swamped too. Since the first wave in 2020, a couple of Sikh religious groups under the umbrella of Covid Fight Support Saanjh (CFSS), a religious charity, have been soliciting oxygen cylinders, beds, even food deliveries using private donations.
“In 2020, when we received around 40 calls for help in a day, we’d worry that our medical infrastructure was getting over-burdened,” says a CFSS member who wishes to stay unnamed. “Today, we received over 1,400 calls, all from people in dire need.”
The COVID-19 resource help desk initiated by Miranda House, a constituent college at the University of Delhi, is equally overworked. “I’ve been fielding between 300-500 calls a day,” estimates BA third-year student volunteer Vitti Joshi. “I start around 6 am and finish in the early hours of the morning and still feel there’s so much more to do.”
Meanwhile, in hospitals, doctors make do with few precious ventilators. “When a patient on a ventilator dies, the focus is first on sterilizing the equipment for the next patient before the body (of the first patient) is taken away,” says Dr. Bhatti. “Usually, the next in line is wheeled in before the (deceased) previous patient is wheeled into the mortuary.”
Medics like Dr. Kafeel Khan in Gorakhpur city in Uttar Pradesh point out that Indian hospitals, dependent on distant oxygen suppliers, have always had shaky oxygen infrastructure. Khan was the nodal officer in charge of the encephalitis ward in the state-run BRD Medical College hospital in Gorakhpur city of Uttar Pradesh in 2017. When the hospital’s piped oxygen supply ran out on August 10, 2017, 70 children and 18 adults died within 48 hours. He was suspended (and subsequently absolved) for negligence and has since been a passionate advocate for better oxygen infrastructure in hospitals.
An invisible fallout
A few weeks into the second wave, doctors, nurses, charities, and patients alike have reported experiencing acute anxiety, insomnia, loss of appetite, and other symptoms.
Rane, who is currently studying the mental health of frontline nurses in Maharashtra, says that such anxiety is compounded by long work hours, poor pay – nurses in the state, for instance, are paid about US$297 a month, and meagre, if any, hazard allowance – as well as having to witness daily deaths.
Doctors are, in some ways, the hardest hit, because in spite of their expertise and training, they’re forced to see patients die on their watch. “All of us are experiencing great despair,” says Dr. Bhatti. “We know that whatever we do, however hard we work, patients are going to keep coming.” Their anxiety is fuelled by the fear that they – and the already broken healthcare system — may not be able to withstand further `waves’ of coronavirus.
Students manning the Miranda House COVID resource help desk are running low on emotional reserves too.
“For every person we are able to help, there are two, sometimes three more equally desperate people that we’re forced to turn away,” says Joshi, the Miranda House student, who is coordinating hospital bed resources. “I think we now need counselling ourselves!”

Maharashtra nurses gather in prayer before going on duty.
A manmade crisis
In the 2021-22 Budget, union finance minister Nirmala Sitharaman announced an increase in the allocation for health by 137 percent to US$30.70 billion. This included budgets for the Ministry of Ayurveda, Yoga and Naturopathy, Unani, Siddha and Homoeopathy (AYUSH); the Department of Drinking Water and Sanitation; National Nutrition Mission under the Ministry of Women and Child Development, among others. A fraction, US$4.80 billion was allocated for the COVID-19 vaccine in 2021-22.
“Given the inadequacies of our medical infrastructure, since last year, we’d been advocating that to break the chain of viral transmission, it was imperative to increase testing and contact tracing and develop proper isolation protocols,” says Dr. Bhatti. Not only did this not happen, India’s vaccine slow rollout (only 2 percent of the population has been fully vaccinated as of May 3) meant that when the second wave struck, the majority of its population was unprotected.
“The government’s misguided decisions to allow ‘superspreader’ events like the Kumbh Mela, mega election rallies in the four Indian states having assembly elections, and Indian Premier League matches across the country directly ensured the spread of the second wave,” he fumes. Dr. Bhatti is not alone in this sentiment. In the last week of April, the hashtag #ResignModi began to trend, reflecting growing public outrage at how Prime Minister Modi’s administration has handled the pandemic.
Human rights advocates say that amid the second wave, the right to life with dignity guaranteed by Article 21 of the Indian constitution is being violated outside every local COVID hospital.
“Our fundamental right to life, and consequently, our right to health care has been violated by the Indian government today,” says human rights activist and former director of Amnesty International India, Avinash Kumar.
“By not providing access to hospitals, oxygen and life- saving drugs, the Indian government has violated our right to life.”
Meanwhile, India became the first country in the world to report over 400,000 new cases in a single day on April 30 and daily infections numbered 368,000 on May 3. Epidemiologists fear this could peak to 500,000 cases daily, potentially with one million deaths from COVID-19, by August this year. By then there may not be enough wood left for funeral pyres. ●
*Name changed on request.
Geetanjali Krishna is a contributing editor with Business Standard and is the co-founder of The India Story Agency, which specializes in telling human interest, environmental, and social affairs stories. Her recent by-lines can be found in Times, BBC, Footprint magazine, and Business Standard.



















